Arrhythmias
 Alternative names
Alternative names
Dysrhythmias; Abnormal heart rhythms; Bradycardia; Tachycardia
Definition
An arrhythmia is any disorder of your heart rate or heart rhythm, such as beating too fast (tachycardia), too slow (bradycardia), or irregularly.
Causes, incidence, and risk factors
Normally, the 4 chambers of the heart (2 atria and 2 ventricles) contract in a very specific, coordinated manner.
The electrical impulse that signals your heart to contract in a synchronized manner begins in the sinoatrial node (SA node), which is your heart's natural pacemaker.
The signal leaves the SA node and travels through the 2 upper chambers (atria). Then the signal passes through another node (the AV node), and finally, through the lower chambers (ventricles). This path enables the chambers to contract in a coordinated fashion.
Problems can occur anywhere along this conduction system, causing various arrhythmias. Examples include:
- Supraventricular tachycardia - a fast heart rate that originates in the upper chambers (atria). The most common are atrial fibrillation or flutter, and atrioventricular nodal reentry tachycardia.
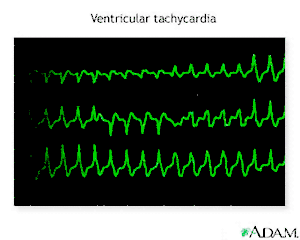
- Ventricular tachycardia - a fast heart rate that originates in the lower chambers (ventricles).
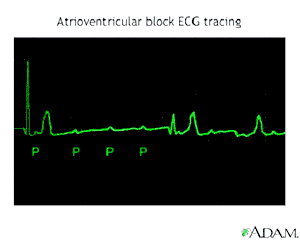
- Bradycardia - a slow heart rate due to problems with the SA node's pacemaker ability, or some interruption in conduction through the natural electrical pathways of the heart.
The risks of getting a tachycardia or bradycardia varies greatly, depending on the condition of your heart, prior heart attack, blood chemistry imbalances, or endocrine abnormalities.
Arrhythmias may also be caused by some substances or drugs, including beta blockers, psychotropics, sympathomimetics, and caffeine. Sometimes antiarrhythmic medications -- prescribed to treat one type of arrhythmia -- can actually cause another type of arrhythmia.
Some types of arrhythmias may be life-threatening if not promptly and properly treated.
 Symptoms
Symptoms
- Fast or slow heart beat (palpitations)
- Skipping beats
- Fainting
- Light-headedness, dizziness
- Chest pain
- Shortness of breath
- Skipping beats - changes in the pattern of the pulse
- Paleness
- Sweating
- Cardiac arrest
The person may not have symptoms.
Signs and tests
A doctor will listen to your heart with a stethoscope and feel your pulse. Your blood pressure may be low or normal.
The following tests may be performed to identify arrhythmias:
- ECG
- Ambulatory cardiac monitoring with a Holter monitor (used for 24 hours) or loop recorder (worn for 2 weeks or longer)
- Echocardiogram
- Electrophysiology study (EPS)
- Coronary angiography
If an arrhythmia is detected, various tests may be done to confirm or rule out suspected causes. EPS testing may be performed to locate the origin of the arrhythmia and determine the best treatment, especially if a pacemaker implantation or catheter ablation procedure is being considered.
Treatment
When an arrhythmia is serious, urgent treatment may be required to restore a normal rhythm. This may include intravenous medications, electrical "shock" therapy (defibrillation or cardioversion), or implanting a temporary pacemaker to interrupt the arrhythmia.
Supraventricular arrhythmias may be treated with anti-arrhythmic drugs. However, most supraventricular arrhythmias can be treated and cured with radiofrequency ablation, eliminating the need for lifelong drug therapy.
Increasingly, many ventricular tachycardias are treated with an implantable cardioverter-defibrillator (ICD). As soon as arrhythmia begins, the ICD sends a shock to terminate it, or a burst of pacing activity to override it.
Bradycardias that cause symptoms can be treated by implanting a permanent pacemaker.
Expectations (prognosis)
The outcome is dependent on several factors:
- The kind of arrhythmia -- whether it is supraventricular tachycardia, or a more dangerous arrhythmia such as ventricular tachycardia or ventricular fibrillation, which are potentially fatal
- The overall pumping ability of the heart
- The underlying disease and its ability to be treated
With bradycardias treated with a permanent pacemaker, the outlook is usually good.
Complications
- Angina (chest pain caused by imbalance of supply and demand for oxygen in the heart muscle)
- Heart attack
- Heart failure
- Stroke
- Sudden death
Calling your GP or cardiologist
Call your doctor if you develop any of the symptoms of a possible arrhythmia. Also call your doctor if you have been diagnosed with an arrhythmia and your symptoms worsen or do not improve with treatment.
Prevention
Taking steps to prevent coronary artery disease may reduce your chance of developing an arrhythmia. These steps include not smoking; eating a well-balanced, low-fat diet; and exercising regularly.
Update Date: 11/6/2006
Updated by: Glenn Gandelman, MD, MPH, Assistant Clinical Professor of Medicine, New York Medical College, Valhalla, NY. Review provided by VeriMed Healthcare Network.
