Stable angina
 Alternative names
Alternative names
Angina - stable; Angina - chronic; Angina pectoris
Definition
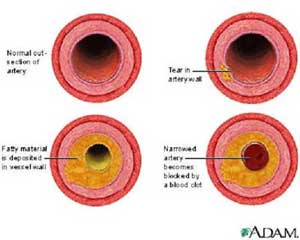
Angina is chest pain caused by too little blood flow to the heart muscle. The pain usually begins slowly and gets worse over a period of minutes before going away. Stable angina typically occurs when you exert yourself, and is quickly relieved with medication or rest. It is also called chronic angina.
Angina chest pain that lasts longer than a few minutes or occurs with rest is considered unstable angina.
Causes, incidence, and risk factors
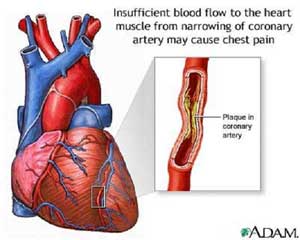
The most common cause of angina is coronary artery disease (CAD). Angina pectoris is the medical term for this type of chest pain.
Situations that increase blood flow to the heart may cause angina in people with CAD. These include exercise, heavy meals, and stress.
The risk factors for angina pectoris include:
- Male gender
- Cigarette smoking
- High cholesterol levels (in particular, high LDL and low HDL cholesterol)
- High blood pressure
- Diabetes
- Family history of coronary heart disease before age 55
- Sedentary lifestyle
- Obesity
Less common causes of angina include:
- Coronary artery spasm (also called Prinzmetal's angina)
- Diseases of the heart valves
- Heart failure
- Abnormal heart rhythms
- Anemia
 Symptoms
Symptoms
Stable angina:
- Occurs after activity, stress, or exertion
- Lasts 1 to 15 minutes
- Is usually relieved with rest or nitroglycerin
The most common symptom is a feeling of tightness, heavy pressure, or squeezing or crushing chest pain that:
- Occurs under the breastbone or slightly to the left
- Is not clearly focused in one spot
- May spread to shoulder, arm, jaw, neck, back, or other areas
- May feel like gas or indigestion
You should seek medical attention if you have new, unexplained chest pain or pressure. If you have had angina before, call your doctor.
Immediately go to the hospital if chest pain or heaviness lasts longer than 15 minutes or is not relieved with medication prescribed by your doctor. The pain may represent unstable angina or a heart attack.
 Signs and tests
Signs and tests
The following tests may be done to diagnose or rule out angina:
- Blood pressure measurement
- Exercise tolerance test (stress test or treadmill test) -- may show ECG changes
- Stress echocardiogram - may reveal problems with the heart's ability to pump blood
- Coronary angiography
- CT angiography
Treatment
The goals of treatment are threefold:
- improve stability and reduce the progression of disease,
- to reduce symptoms and
- to prevent complications.
There are three primary forms of medication for stable angina.
- Medications that improve long-term health include cholesterol-lowering drugs like Lipex or Lipitor. These and other cholesterol lowering drugs are the most powerful agents against the generally progressive and unpredictable nature of coronary artery disease. They work by reducing the fat content of plaques that obstruct arteries. The reduction is fat stabilises the artery making it less prone to rupture and potentially deadly myocardial infarction. It is perhaps through this mechanism that lipid lowering agents have been found to be the only drugs to reduce mortality (or improve survival) in patients who suffer from angina. No other class of drugs comes close to their effectiveness.
- The second mechanism of effectiveness is by reducing progression of disease i.e. the blockages are less likely to progress, particularly if the LDL is reduced sufficently with an adequate dosage of tablets.
Other drugs that help reduce complications include aspirin and clopidogrel (Plavix). These drugs do not reduced mortality in angina, but are important in reducing complications such as myocardial infarction and stroke.
Medications that improve symptoms include nitrates, calcium channel blockers and beta blockers. These drugs work through different mechanisms to reduce the effort that the heart has to expend in pumping blood around the body.
However, if you experience angina pain, you should:
Rest
Take nitroglycerin spray or tablet
Your doctor may recommend a cardiac rehabilitation program to help improve your heart's fitness.
Some patients may need cardiac intervention such as:
Percutanueous Transluminal Coronary Angioplasty (PTCA) and stenting or,
Coronary artery bypass grafting (CABG)
 Expectations (prognosis)
Expectations (prognosis)
Stable angina usually improves with medication.
Complications
Unstable angina
Heart attack
Sudden death caused by lethal arrhythmias
Contact your GP if you are concerned or if you have the above symptoms
Call your health care provider if any of the following occur:
Chest pain develops that has not been evaluated
Your angina changes in frequency, severity, duration, or character (for example, it happens at rest or lasts longer than 15 minutes)
Your angina requires increasing doses of nitroglycerin
Prevention
Your doctor may tell you to take nitroglycerin a few minutes in advance if you plan to perform an activity that may trigger angina pain.
The best prevention for angina is to lower your risk for coronary heart disease.
Stop smoking
Lose weight if you are overweight
Control blood pressure, diabetes, and cholesterol
Reducing risk factors may prevent the blockages from getting worse and can reduce their severity, which reduces angina pain.
References
U.S. Food and Drug Administration. FDA Approves New Treatment for Chest Pain. Rockville, MD: National Press Office; January 31, 2006. Press Release P06-15.
Zipes DP, Libby P, Bonow RO, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, 7th ed. St. Louis, Mo; WB Saunders; 2005: 1281-1308.
Mehta SB. Management of coronary heart disease: stable angina, acute coronary syndrome, myocardial infarction. Prim Care. 2005; 32(4): 1057-81.
