- Home
- Our services
- Consultations
- Diagnostics
- Intervention
- Angioplasty and stenting
- Stent Animation
- Heart bypass surgery
- A guide to angioplasty (PDF)
- A guide to bypass surgery (PDF)
- Cardioversion
- Cardiac Pacemaker
- Implantable Cardiac defibrillators
- Radiofrequency ablation
- Heart valve surgery
- Valve repair surgery
- Mechanical valve replacement
- Tissue valves
- Guided Imagery
- Heart Surgery Recovery
- Heart Valve Types
- Education
- Our Mission
- Search
- Contact
Cardiac Pacemaker
 Reasons for Pacemaker Implantation
Reasons for Pacemaker Implantation
Almost all pacemakers are implanted to treat slow heart beating, which is called "bradycardia." At rest, the heart usually beats about 50 to 70 times each minute, and the heart rate may increase 2- to 3-fold during stress or exercise. If the heart beats too slowly, the brain and body do not get enough blood flow and a variety of symptoms may result.
Symptoms Associated With Need for a Pacemaker
- Fainting
- Near fainting
- Dizziness
- Lack of energy
- Fatigue
- Shortness of breath
- Exercise intolerance
Extreme slowing or complete stopping of the heartbeat can be fatal. In other cases, people may have no symptoms but are at high risk for dangerously slow heart rates because of disturbances of the electrical system of the heart. A pacemaker may be recommended for these people before symptoms occur.
The normal heartbeat is controlled by a natural pacemaker in the heart called the sinus node. The electrical signal generated by the sinus node spreads throughout the heart causing it to beat. The most common reason for pacemaker implantation is because the sinus node function becomes too slow from age, heart disease, or heart medications. The other leading cause for pacemaker implantation is failure of the normal electrical signal to reach the main pumping chambers, causing the slow heart rate known as heart block. The artificial pacemaker implanted by cardiologists corrects both causes of slow heart beating by providing electrical signals to tell the heart to beat at the proper rates and by delivering the signal to the appropriate chambers of the heart.
The Pacemaker and Its Implantation

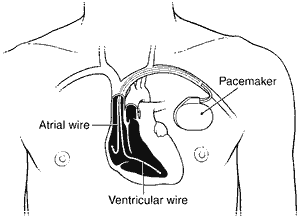
The pacemaker system includes the pacemaker itself and wires that connect the pacemaker to the heart. The pacemaker unit is slightly larger than a man’s wristwatch and contains a battery and computer circuits (Figure 1). The computer circuits perform the functions of monitoring the patient’s underlying heart rhythm and delivering an electrical signal to cause the heart to beat at the desired rate. Many pacemakers implanted today also may have rate responsiveness features that allow temporary pacing of the heart at faster rates during periods of exercise. Single-chamber pacemakers have only one wire connected to the heart and dual chamber pacemakers have wires to both the top and bottom chambers of the heart (Figure 2). Your cardiologist will recommend which type of pacemaker is needed.
The pacemaker is implanted by a minor surgical procedure performed under local anesthesia. The wires are placed through a blood vessel beneath the collar bone and positioned in the heart under x-ray. The wires are then connected to the pacemaker, which is placed beneath the skin just below the collar bone. The surgery usually takes about 1 to 2 hours, and the risk of surgical complications is about 1% to 2%. Usually only a small bump in the skin is seen over the place where the pacemaker has been implanted. Other than restrictions on heavy lifting and extreme motion of the arm on the side of the pacemaker for several weeks, recovery from the procedure is minimal. Most patients return to normal activities within a few days. It is recommended that patients carry an identification card that provides specific information on the type of leads and pacemaker implanted. Such a card can be shown to healthcare professionals during medical evaluations and to security personnel at airports.
What to Expect After the Pacemaker
After the pacemaker is implanted, it should be evaluated by your cardiologist or the cardiac technetian every 3 to 6 months with the use of a computer that will provide information about how the pacemaker is working and about the life of the battery. Such periodic checks on the battery usually give a several-month warning before the pacemaker requires replacement because of low battery voltage. The average pacemaker battery lasts about 5 to 8 years. Some people may be advised to have their pacemakers checked monthly over the telephone (known as telephonic surveillance). In the vast majority of patients, the presence of the pacemaker does not change lifestyle or activities in any way. Your cardiologist will review any possible restrictions with you. There are some situations, however, that are to be avoided if you have a pacemaker, such as full-contact sports, which may damage the pacemaker, exposure to arc welding equipment, magnetic resonance scanners (MRI), and high-voltage commercial transformers.
Common Misconceptions About Pacemakers
People have many misconceptions about pacemakers arising from popular notions or outdated information. Always ask your cardiologist if you have any questions about your pacemaker. The following are the most common misconceptions:
- "With my pacemaker I cannot use a microwave oven." This was true for very old pacemakers but is not true today. People with pacemakers may use all types of household appliances and power tools.
- "With my pacemaker I cannot use a cellular telephone." Although there is a possibility of interference with some high-power digital cell phones, people with pacemakers usually need only to keep the phone out of clothing pockets near the pacemaker and hold the phone to the ear away from the pacemaker.
- "With my pacemaker I will have to slow down." This is false. In our practice, we have pacemaker patients who play sports such as golf, tennis, or basketball. Pacemaker patients can even participate in more strenuous activities such as marathons or scuba diving after consultation with their cardiologists. Any activity restrictions usually result from other medical problems and not from the pacemaker.
- "With my pacemaker I cannot travel." By always carrying the identification card given at the time of the pacemaker implantation, patients can have their pacemaker evaluated in almost any part of the world if needed. It is also safe to pass through airport security checks in the normal fashion.
- "With my pacemaker I won’t need heart medications." The pacemaker does not replace the need for heart medications to treat high blood pressure, angina, heart rhythm problems, etc. Most people with pacemakers also take heart medications.
- "I have a pacemaker, so I cannot have a heart attack." The pacemaker does not protect against blockages in blood vessels that cause heart attacks. Similarly, people may still have fast heart rhythm problems that the pacemaker cannot treat directly. The standard pacemaker does not strengthen the heart, although some new types of pacemakers may be helpful in certain patients with congestive heart failure. With pacemaker implants, patients should continue to follow a heart-healthy lifestyle that includes exercise, diet, and cardiac medications when prescribed.
Additional Information
Additional information about pacemakers is available from the following sources:
- The American Heart Association at http://www.americanheart.org
- The North American Society of Pacing and Electrophysiology at http://www.naspe.org
- Pacemaker Club at http://www.pacemakerclub.com
- WebMD at http://www.WebMD.com
- For information on another commonly implanted device, the implantable cardioverter-defibrillator (ICD), see the Cardiology Patient Page by Reiffel and Dizon, "The Implantable Cardioverter-Defibrillator: Patient Perspective," which was published in the March 5, 2002, issue of Circulation (Circulation. 2002;105:1022–1024).
